Health Optimisation Medicine is a proactive, data-driven approach to care that aims to keep you well—rather than only treating you once you are sick. Instead of waiting for symptoms, it looks at early signals in your biology (from routine labs to advanced biomarkers), your daily habits, and your environment.
The goal is simple: create personalised plans that help your body function at its best, so you feel better today and build resilience for tomorrow. This approach complements conventional medicine by filling the prevention gap, guiding smarter lifestyle choices, and aligning care with what matters most to you—energy, focus, sleep, and long-term health.
In real-world settings, Health Optimisation Medicine and Practice turns principles into repeatable workflows. A typical journey starts with an in-depth assessment: history, goals, sleep and stress patterns, movement, nutrition, and targeted blood work. Where appropriate, clinicians may integrate wearable and at-home data to understand trends, not just one-off results. From there, a practitioner designs a personalised plan focused on foundations—nutrition quality, micronutrient status, gut and metabolic health, movement, recovery, and stress regulation—before layering targeted interventions if needed.
Follow-up is structured and iterative. Patients review progress at defined intervals, update labs when relevant, and adjust plans in small, sustainable steps. Education is central: you learn why a recommendation exists, how to implement it in daily life, and what to track to recognise improvements. Collaboration with your existing healthcare providers is encouraged, ensuring safety, coordination, and continuity—especially if you live with chronic conditions or take prescription medications. Over time, this practice model builds a living profile of your health so care becomes more precise and more effective with each cycle.
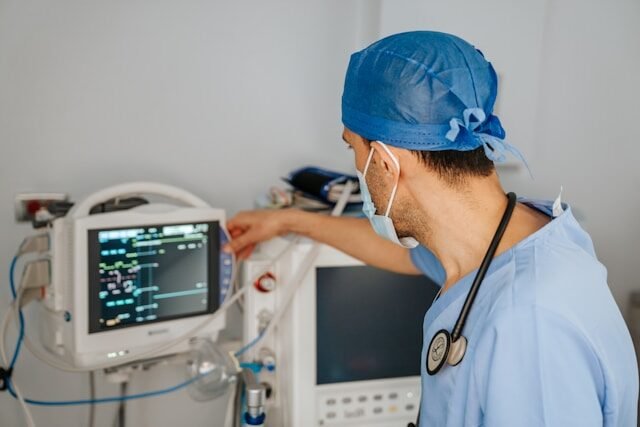

Medicine optimisation focuses on using the right interventions for the right person at the right time—and minimising anything unnecessary. In prevention-focused work, that often means optimising lifestyle “prescriptions” first: protein and fibre intake, hydration, circadian-friendly routines, resistance and aerobic training, and stress-recovery balance. Where supplements or medications are appropriate, they are selected for quality, dosing, and interactions, then reviewed regularly for benefit–risk and ongoing need.
This optimisation lens also applies to testing. The aim is not to run every panel available but to choose markers that inform decisions: metabolic health (glucose, lipids), inflammation and recovery, nutrient status, and—when indicated—hormonal balance or gut function. Results are interpreted in context: your symptoms, goals, age, sex, activity levels, and preferences. The outcome is a plan that is lean, targeted, cost-aware, and easier to follow—making long-term adherence more likely and results more durable.
Prevention as the default. It emphasises early detection and course-correction before issues escalate.
Personalisation built on data. Objective measures and lived experience guide your plan together.
Behaviour change that sticks. Practical steps, tracking, and feedback loops help turn good intentions into habits.
Collaboration across disciplines. Clinicians, coaches, nutritionists, and specialists coordinate around your goals.


Busy professionals seeking better energy, focus, and stress resilience.
Athletes and active people wanting performance without burnout.
People managing risk (family history, metabolic concerns) who prefer proactive care.
Anyone who believes health is more than “not being sick” and wants a clear framework to improve it.
Assess: Comprehensive intake, goal-setting, baseline labs, and lifestyle snapshot.
Plan: Personalised recommendations across nutrition, movement, sleep, stress, and, when useful, targeted supplementation.
Act: Simple weekly actions, educational resources, and optional digital tracking.
Review: Regular check-ins to evaluate progress and refine the plan.
Sustain: Long-term rhythm with periodic re-testing and habit maintenance.

When Health Optimisation Medicine is implemented well, people often report steadier energy, deeper sleep, improved body composition, better mental clarity, and fewer “off” days. These are meaningful quality-of-life gains. Just as importantly, the approach helps you build literacy about your own health—what to watch, how to respond, and when to seek further care. It does not replace your primary physician; it makes every interaction with the healthcare system more informed and effective.
If you’re ready to move beyond one-size-fits-all advice, Health Optimisation Medicine offers a structured, personalised pathway to feel and function at your best. Start with a clear baseline, choose the smallest changes that create the biggest wins, and iterate. Your health is dynamic—your plan should be, too.